The Connection between “Tamper-Resistant” Opioids and Skyrocketing Communicable Disease Crises

Opioid painkillers are a class of drugs which started off seeming like a good idea but which instead ended up creating the worst addiction epidemic that our nation has likely ever seen. Opioid painkillers saw their major debut in the late-1990s, but within five to ten years, millions of Americans were addicted to them and thousands had died from overdoses.
Mass public outrage turned against the pharmaceutical organizations which made the drugs and which had promised us that opioid analgesics were “safe and addiction-free.” What a lie that was. And to redirect public outrage (and some grievous lawsuits as well) Big Pharma did the only thing they knew how to do. They released a new line of opioid painkillers which were, lo and behold, “abuse-deterrent!”
The idea behind abuse-deterrents was to create pharmaceutical pills which would be more difficult to crush into a powder, i.e. making them more difficult to snort or dissolve in water and inject. Furthermore, abuse deterrents were enhanced with a special formula that, even if a drug user did manage to crush them somehow and then dissolve them in water for IV use, the drug would become pasty, a sort of gummy sap that would not be injectable. The end result was technically successful. New abuse-deterrents were very difficult to crush into a powder or dissolve. The goal on pharma manufacturers’ plan was to make pills that drug users could neither snort or inject, (or which, at least, would be far more difficult to use in those ways).
But that plan backfired, because instead of curbing the opioid addiction epidemic, the proliferation of abuse-deterrents into the pain reliever market simply forced addicts to seek out other hard drugs like heroin and illicitly manufactured synthetic opioids. IV opioid misuse soared, and suddenly the instances of communicable diseases increased in tandem.
That’s right. A direct result of pharmaceutical organizations releasing abuse-deterrent opioids was that IV drug use increased and the nation faced a new surge of infectious disease like hepatitis C and HIV.
A Poor “Solution” That Did More Damage Than Good
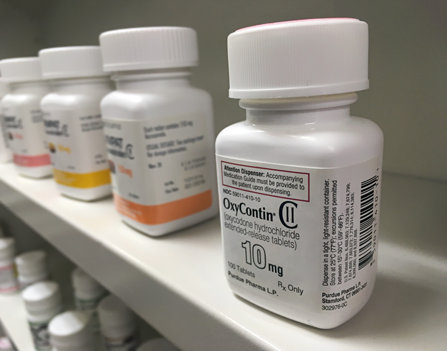
U.S. News reported on the insidious relationship between the introduction of abuse-deterrent (also called tamper-resistant) opioid pain relievers and the increase in both IV drug use and instances of infectious disease. The author, Steven Reinberg, sums up quite eloquently how an effort on behalf of pharmaceutical companies like Purdue Pharma to make opioid drugs like OxyContin more difficult to misuse drove patient-addicts to heroin and other “street opioids” which in turn prompted an increase in hepatitis C infections.
“The fact that we are seeing a rise in hepatitis C infection rates suggests that even if we could stop fatal overdoses, we’re going to have long-term public health consequences because hepatitis C has long-term and very costly effects… .”
The U.S. News article quotes David Powell, senior economist and researcher at the RAND Corporation: “The fact that we are seeing a rise in hepatitis C infection rates suggests that even if we could stop fatal overdoses, we’re going to have long-term public health consequences because hepatitis C has long-term and very costly effects. These results should steer the public and policymakers to increasing access to [Addiction] treatment. If more treatment were available, maybe we could shift more people into treatment than into illicit drug markets.”
I appreciate what David Powell said. His words necessitated a direct quote in this text because his message hits the nail on the head of what we need when it comes to the opioid crisis. We need safer approaches to pain relief, and we need addiction treatment for those currently addicted. It’s not that complicated.
Powell’s research team found that in the months following the reformulation of OxyContin, states which had traditionally high rates of OxyContin abuse were now experiencing increasing rates of hepatitis C infections. In fact, the states were seeing an increase in hepatitis C infections at a rate three times faster than in other states that had not been as harshly affected by OxyContin addiction.
States which already had a high-rate of OxyContin misuse saw an increase of 222 percent in hepatitis C infection in the years following OxyContin reformulation. States with lower OxyContin misuse rates saw only a 75 percent increase in hepatitis C infections in that same period.
Also according to the research, hepatitis C infections had been more or less unchanged for years in the U.S. (until the reformulation of OxyContin, of course). When OxyContin was reformed into an abuse-deterrent drug in 2010, hepatitis C infections soared. Twenty-thousand people died from the disease in 2015. And the result of non-lethal infections? Now infected addicts needed treatment for both opioid addiction and hepatitis C. According to these numbers it seems like the reformulation of OxyContin made the health situation worse, not better.
Had Purdue Pharmaceuticals instituted non-opioid based pain relief options in 2010, we might not be contending with a surge in both IV drug use and hepatitis C infections. Purdue should have innovated a medical solution that provided pain relief while also serving to bring OxyContin users down off of OxyContin—if such a solution is physically possible. Many of the individuals who shifted from OxyContin to hard drugs were “patient-addicts,” individuals who had legitimate pain conditions but who had also fallen prey to chemical dependency to OxyContin. The abuse-deterrent version was not doing it for them. They needed something different, so they explored other options, and they suffered for it. Had Purdue offered a better solution in the first place, likely none of that would have happened.
Reducing Our Reliance on Opioid Pain Reliever Drugs Is the Answer

When pharmaceutical giants offered “abuse-deterrent” drugs to American patients, we were not fooled. Such an effort was more of an act to divert attention off of them for the part they played in the opioid epidemic than it was a legitimate effort to curb opioid addiction. Abuse-deterrents are still addictive. We clearly can no longer place our trust and faith in pharmaceutical organizations to reverse the opioid epidemic. This is a task that we must take on ourselves. We have to mobilize as communities to curb opioid addiction.
Opioid addiction in the U.S. is the worst it has ever been. It is a drug problem that by itself exceeds the dire risks and dangers of all other U.S. drug problems combined. If we don’t take back our cities and rural communities from the opioid crisis now, we may never have a chance to do so again. The death toll, the spread of infectious diseases, the crime and the despair will all continue if we don’t do something about it.
The answer lies in reducing our reliance on opioid pain relievers. We are totally in control of this problem because the problem would not exist were it not for us, the American citizenry. We have to demand alternative solutions to pain relief. Such alternatives do exist, yet they are highly under-publicized due to Big Pharma’s monopoly on medicine.
We have to force ourselves to turn our backs on quick and easy pain relief, as hard as that might be to do. We got on just fine for decades without instant pain relief within arm’s reach. We can do this again. We have to. The fate of our nation depends on it.
According to the Centers for Disease Control and Prevention, more than 702,000 Americans have died from drug overdoses since 1999. Ten percent of them lost their lives in 2017 alone. Most of those deaths have been opioid deaths. When will it stop? The truth is, it won’t stop until we make it stop. Let’s end the opioid trap for good.
Sources:


 ®
®